A new approach to prevent infections in vulnerable people could radically reduce the need for antibiotic treatment
Peter Bergman, one of the researchers that has received funding from PAR Foundation, is investigating how novel compounds could trigger the immune response to treat or even prevent infections. This approach has potential to dramatically reduce the need for antibiotic treatment and a very low risk of driving resistance.
The development of antibiotic resistance is most often linked to misuse of antibiotics, when drugs are used in an unhelpful or unnecessary way, but the fact is that even proper and justified antibiotic use cause bacteria to develop resistance. This aspect tends to get less attention than misuse, probably because it is perceived as difficult to do anything about. When a patient really needs antibiotic treatment, we clearly do not want to withhold it.
If we want to address proper antibiotic use as a driver of resistance, there are however two underlying factors that we can target: firstly, we could try to provide other treatment options, and secondly, we could try to decrease the occurrence of infections. This is exactly what Peter Bergman’s research group at Karolinska Institutet, which has received funding by PAR Foundation, is aiming at.
To understand Peter’s research, we have to take a look at a component in the immune system called antimicrobial peptides, or AMPs for short. AMPs are a part of the innate immune response and function as a natural, broad-spectrum antimicrobial that can kill or destroy bacteria, viruses, and fungi. They were first described in 1981 and now over 2000 AMPs have been identified, and many of them play a part in the human immune system.
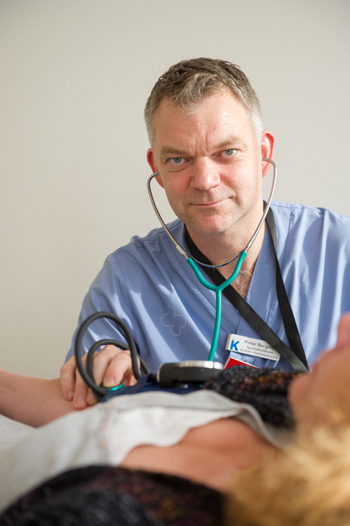
Peter Bergman, researcher and senior physician at Karolinska Institutet, is one of the grantees of PAR Foundation
The most straightforward approach would be to pick some of these potent AMPs and turn them directly into an antimicrobial drug for infection treatment. Peters’ research, however, is using a more subtle approach: he studies novel compounds that can be used to trigger the body’s own production of AMPs.
– These compounds we are looking at are much more feasible to use than AMPs directly – they are more stable and could be turned into pills or creams or sprays or whatever formulation you would want, and they are also easy to produce, meaning the product would be very scalable.
The project is run in collaboration with a group of Icelandic researchers, and there is an associated start-up company, Akthelia, that is aiming to turn this research into novel drugs.
The research results show that these compounds can make a resistant infection treatable again with first-line antibiotics, meaning that they could be used in combination with first-line antibiotics to treat resistant infections. But there is also the possibility of pursuing this as a stand-alone treatment for infections, reducing the need for antibiotics.
The compound could even be used to prevent infections before they occur. Preventive treatment could be particularly interesting for vulnerable groups such as elderly, immunosuppressed or cancer patients that are particularly susceptible to infections. Preventive use could also be valuable for healthy individuals that temporarily experience a higher infection risk – at the beginning of the school-year, say, or when taking an intercontinental flight.
An important feature of this kind of treatment is that the risk of driving resistance is particularly low. Studies have indicated a low risk for resistance development for AMP treatments, and triggering the body’s own AMP production rather than inserting a specific AMP reduces this risk even further. This way, it is not one but a multitude of different AMPs that are produced simultaneously, and the likelihood that the bacteria could develop resistance to all of them simultaneously is extremely low.
Peter Bergman emphasises the importance of funding for unconventional research approaches:
– The support of PAR Foundation has been very important for us to be able to do this research. The field of antibiotic resistance and the immune system research is conventionally kept apart, but to achieve new breakthroughs it is important that we dare to think in new ways and combine the knowledge of different fields.
“The field of antibiotic resistance and the immune system research is conventionally kept apart, but to achieve new breakthroughs it is important that we dare to think in new ways and combine the knowledge of different fields.
Related articles
New collaboration between PAR Foundation and the Global AMR R&D Hub
– The collaboration with PAR Foundation is an excellent example for how the Dynamic Dashboard and the work of the Global AMR R&D Hub can support funders and stakeholders in the AMR R&D field more broadly, says Dr Elmar Nimmesgern, who leads the work of the Global AMR R&D Hub from their offices in Germany.
Opinion: Resistance could pose the greatest threat to our health
Debate article by The Foundation to Prevent Antibiotic Resistance, published in one of Sweden’s major daily newspapers Svenska Dagbladet 18 November 2020.
How should we measure our impact?
The Foundation to Prevent Antibiotic Resistance has joined the Swedish impact measurement network Effektfullt, a partner network of Social Value International. We will work together with other change-making organizations to develop effective ways to measure our impact.
